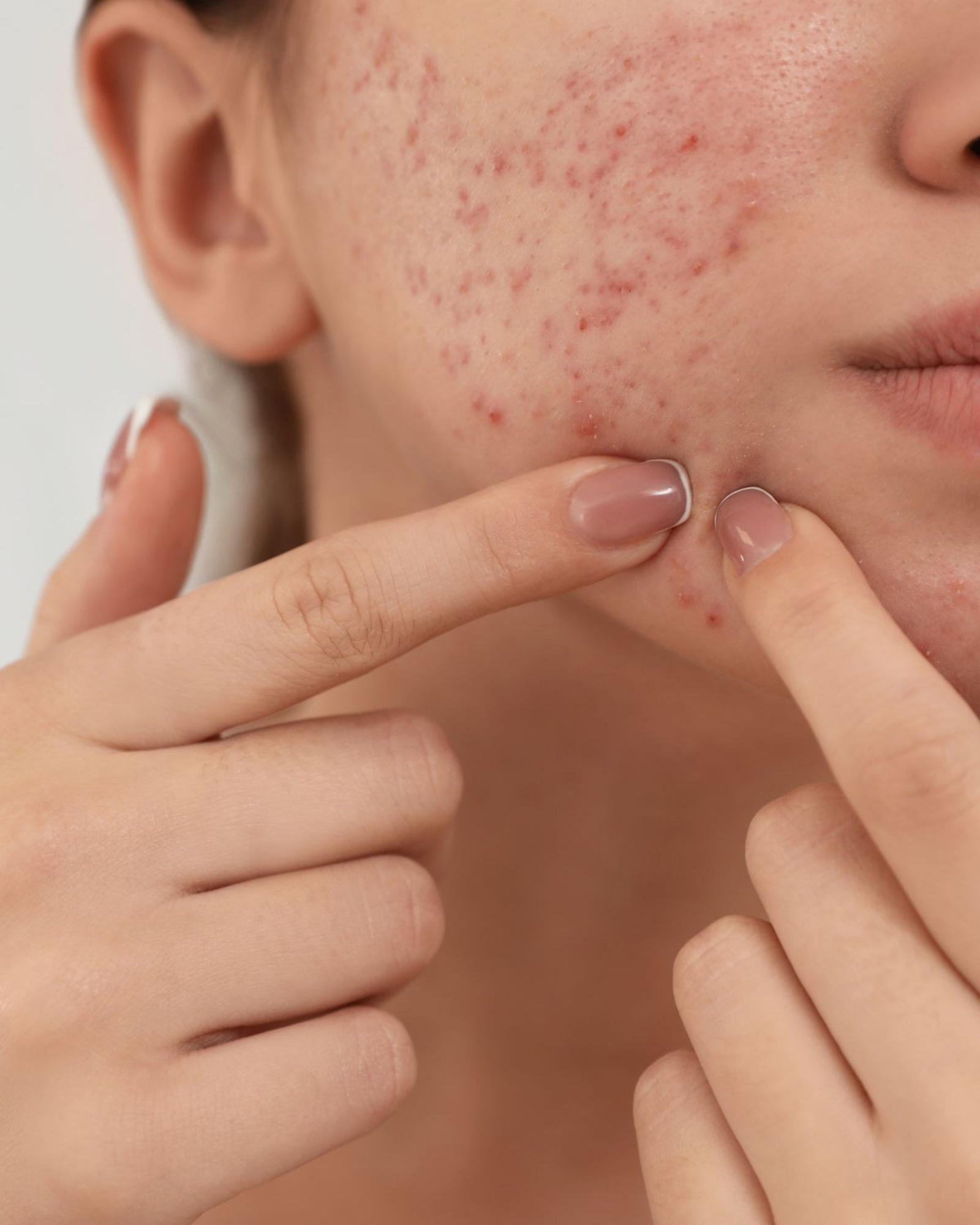
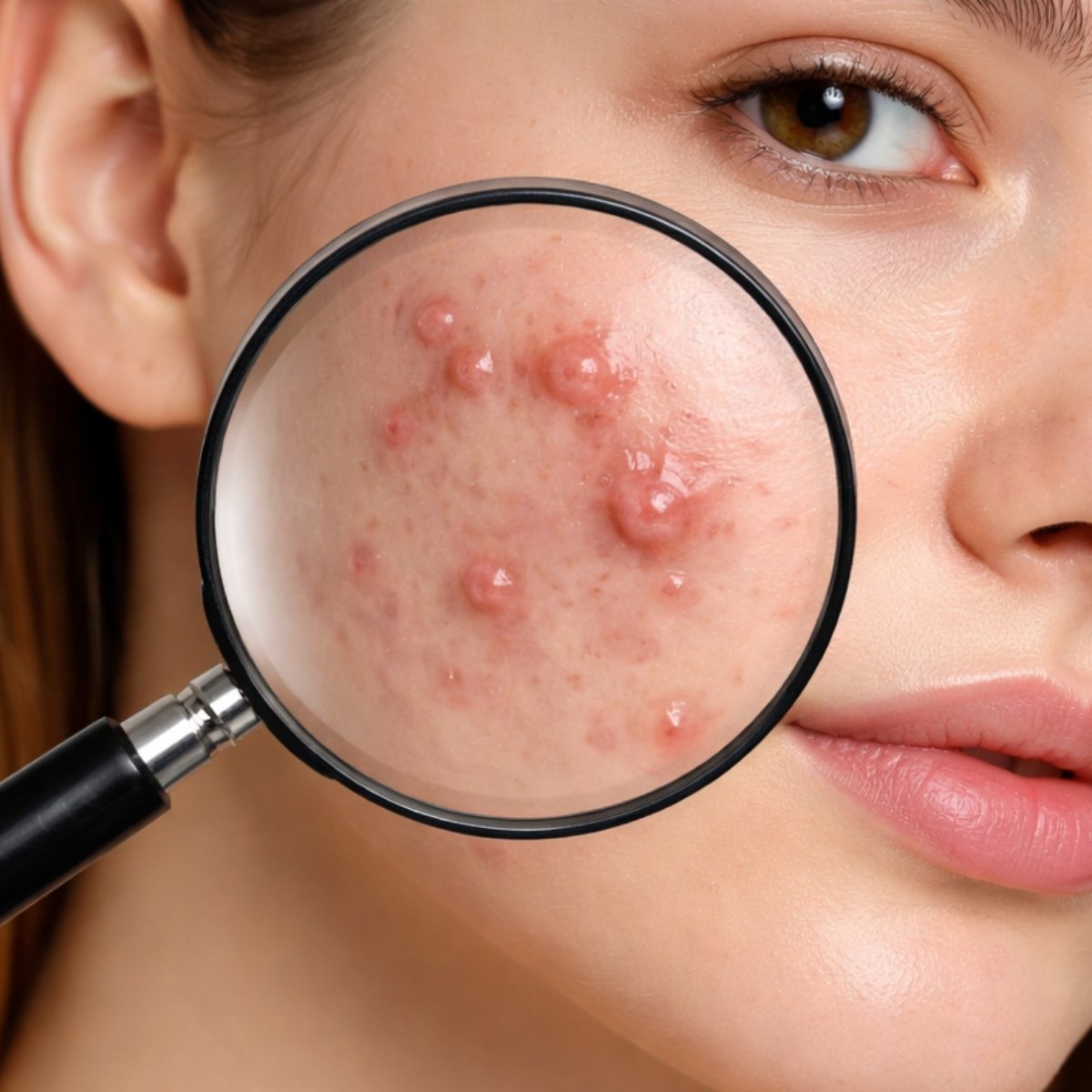
Fungal acne is one of the most misdiagnosed skin conditions.
Many people think they have acne. They use acne treatments like salicylic acid or benzoyl peroxide. But nothing improves.
That’s because fungal acne is not true acne.
Its medical name is Malassezia folliculitis, and it is caused by yeast — not bacteria.
In this guide, we will explain:
-
What fungal acne is
-
What fungal acne looks like
-
What triggers fungal acne
-
What fungal acne feeds on
-
How to tell if acne is fungal or bacterial
-
What fungal acne can be mistaken for
Let’s start with the basics.
What Is Fungal Acne?
Fungal acne is a yeast infection of the hair follicles.
It is caused by an overgrowth of a fungus called Malassezia, which naturally lives on human skin.
Under normal conditions, this yeast does not cause problems. But when it overgrows, it infects the hair follicles and creates inflamed bumps that resemble acne.
Unlike regular acne, fungal acne:
-
Is not caused by clogged pores alone
-
Is not primarily caused by bacteria
-
Does not respond well to typical acne medications
The correct medical term is Malassezia folliculitis.
What Does Fungal Acne Look Like?
One of the most searched questions is: What does fungal acne look like?
Fungal acne usually appears as:
-
Small, uniform red bumps
-
Skin-colored or slightly inflamed bumps
-
Clusters of similar-looking pimples
-
Often itchy
-
No blackheads or whiteheads
The key sign is uniformity. All bumps tend to look the same size and shape.
Regular acne usually shows mixed lesions — blackheads, whiteheads, papules, and pustules together.
Fungal acne does not.
Does Fungal Acne Appear Suddenly?
Yes, it can.
Many people notice fungal acne appearing suddenly, especially after:
-
Long-term antibiotic use
-
Hot, humid weather
-
Excessive sweating
-
Using heavy or oily skincare products
If small, itchy bumps suddenly appear on the forehead, chest, or back and do not improve with acne treatments, fungal acne may be the cause.
What Triggers Fungal Acne?
Several factors can trigger yeast overgrowth.
Heat and Humidity
Malassezia grows more rapidly in warm, humid environments.
Sweat
Sweat trapped under tight clothing creates a moist environment ideal for fungal growth.
Antibiotics
Antibiotics kill bacteria. When bacteria levels drop, yeast can multiply more easily.
This is why fungal acne can develop after acne antibiotic treatment.
Oily Skin
Malassezia feeds on lipids (oils) found in sebum.
More oil means more nutrients for the yeast.
Heavy Skincare Products
Thick creams and oil-based products may worsen fungal acne.
What Does Fungal Acne Feed On?
Malassezia feeds on lipids, especially fatty acids present in human sebum.
It does not feed on sugar from your diet.
Instead, it thrives in oil-rich environments on the skin.
This is why fungal acne commonly appears in areas with higher oil production, such as:
-
Forehead
-
Chest
-
Upper back
-
Shoulders
Fungal Acne vs Regular Acne
Understanding the difference is essential.
| Feature | Fungal Acne | Regular Acne |
|---|---|---|
| Cause | Yeast (fungus) | Bacteria + clogged pores |
| Itching | Common | Rare |
| Lesion type | Uniform bumps | Mixed lesions |
| Blackheads | Usually absent | Common |
| Response to acne treatment | Poor | Usually improves |
| Triggered by antibiotics | Sometimes | Often treated by antibiotics |
If your bumps are itchy and not responding to acne medication, fungal acne should be considered.
Fungal Acne vs Eczema
Eczema usually presents as:
-
Dry, scaly patches
-
Cracked or flaky skin
-
Intense itching
-
Skin thickening over time
Fungal acne presents as:
-
Small similar bumps
-
Inflamed follicles
-
No dry scaling patches
They are clinically different conditions.
Fungal Acne or Perioral Dermatitis?
Perioral dermatitis typically:
-
Appears around the mouth
-
Causes red rash-like clusters
-
May burn or sting
-
Is often triggered by topical steroids
Fungal acne:
-
Commonly affects forehead, chest, and back
-
Causes uniform itchy bumps
-
Is not limited to the mouth area
Location and symptoms help differentiate them.
Can Fungal Acne Cause Cysts?
No.
Fungal acne does not usually cause deep cysts or nodules.
Large, painful cysts are typically associated with severe inflammatory or hormonal acne.
If deep, painful lumps are present, it is more likely cystic acne rather than fungal acne.
What Can Be Mistaken for Fungal Acne?
Conditions that may look similar include:
-
Closed comedones
-
Heat rash
-
Milia
-
Bacterial folliculitis
-
Perioral dermatitis
-
Eczema
Because fungal acne resembles other small bump conditions, proper diagnosis may require medical evaluation.
How to Tell If Acne Is Fungal or Bacterial
You may suspect fungal acne if:
-
The bumps are itchy
-
All bumps look similar
-
It worsened after antibiotic use
-
It appears mainly on forehead, chest, or back
-
Acne products are not helping
However, a dermatologist can confirm the diagnosis more accurately.
Brief Note on Treatment
Since this article focuses on types of acne, treatment will be kept brief.
Fungal acne requires antifungal treatment.
Typical acne medications alone may not work.
Medical options may include:
-
Topical antifungal creams
-
Medicated antifungal washes
-
Oral antifungal medication in persistent cases
Proper diagnosis is essential before starting treatment.
Final Summary
Fungal acne, medically known as Malassezia folliculitis, is a yeast-related infection of hair follicles that mimics acne but behaves differently. It appears as small, uniform, often itchy bumps and is commonly triggered by heat, sweat, antibiotics, and oily skin. Unlike regular acne, it does not respond well to traditional acne treatments because the underlying cause is fungal, not bacterial. Understanding the difference between fungal acne and regular acne is important for proper management and avoiding unnecessary irritation.